Written and clinically reviewed by Cheryl Groskopf, LMFT, LPCC
Trauma-informed Somatic & IFS Therapist
Cheryl Groskopf is a dual-licensed LMFT and LPCC in Los Angeles, specializing in anxiety, trauma, and nervous system–informed therapy for high-functioning adults. Her work focuses on helping clients understand stress responses, reconnect with their bodies, and move out of survival mode through somatic and trauma-informed approaches.
Last updated: December 28, 2025
What Does It Mean to Shut Down Under Stress?
Shutting down under stress is a protective nervous system response. When stress feels too intense or ongoing, the body may move into a freeze or shutdown state to reduce overwhelm. This can look like numbness, mental fog, low energy, or feeling disconnected, even when life appears “fine.”
Table of Contents
Why Shutdown Happens Under Chronic Stress
When people hear the word shutdown, they often picture something extreme (i.e. collapsing, disappearing, or completely checking out). But shutdown is usually much quieter than that. It’s the nervous system easing off the gas when it no longer believes effort will help.
Fight and flight require energy. They assume there’s something you can do. Shutdown shows up when the system decides doing more isn’t safe or sustainable. So sensation dulls. Motivation drops. Focus narrows.
This pattern is especially common in people who stayed functional under chronic pressure. You kept showing up. You handled what needed to be handled. You didn’t fall apart when it would’ve made sense to. Shutdown often arrives after the crisis, once your system finally has permission to stop pushing.
This kind of stress response aligns with how the brain and nervous system adapt to prolonged threat, as described by the National Institute of Mental Health in its overview of trauma and stress-related conditions.
Why This Makes Sense
When stress lasts too long or feels impossible to escape, the nervous system shifts into conservation mode. It’s a survival response designed to reduce overload when other survival options feel unavailable.

How Shutdown Shows Up in High-Functioning Adults
Shutdown doesn’t always look like falling apart. In high-functioning adults, it’s often internal, meaning it’s harder to spot, easier to dismiss, and easier to judge yourself for.
You might still be getting through the day, meeting responsibilities, and showing up for others. But internally, everything feels heavier. Tasks that used to be easy now require a disproportionate amount of effort. Decisions feel draining. Your body feels distant or muted. You’re not hyped up “anxious” in that sense, but you certainly feel…less available.
This is where people get confused. If you’re not panicking, you assume you must be calm. But shutdown isn’t calm. It’s low-energy protection.
You Might Notice
- Your body feels heavy or slow to respond, especially in the morning
- Thinking feels foggy, blank, or effortful
- Small tasks suddenly feel overwhelming or impossible to start
- You want to withdraw rather than explain what’s going on
- Emotion feels muted or “flat”
Try This (If You’re Reading This While Shut Down)
You don’t need to change anything right now. Just notice where your body is making contact with what’s supporting it — the chair, the floor, the couch beneath you. Let your attention rest there for a few seconds. No fixing. No deep breaths. Just noticing support.
Why this works: Passive orientation lowers threat without asking your nervous system to mobilize before it’s ready.
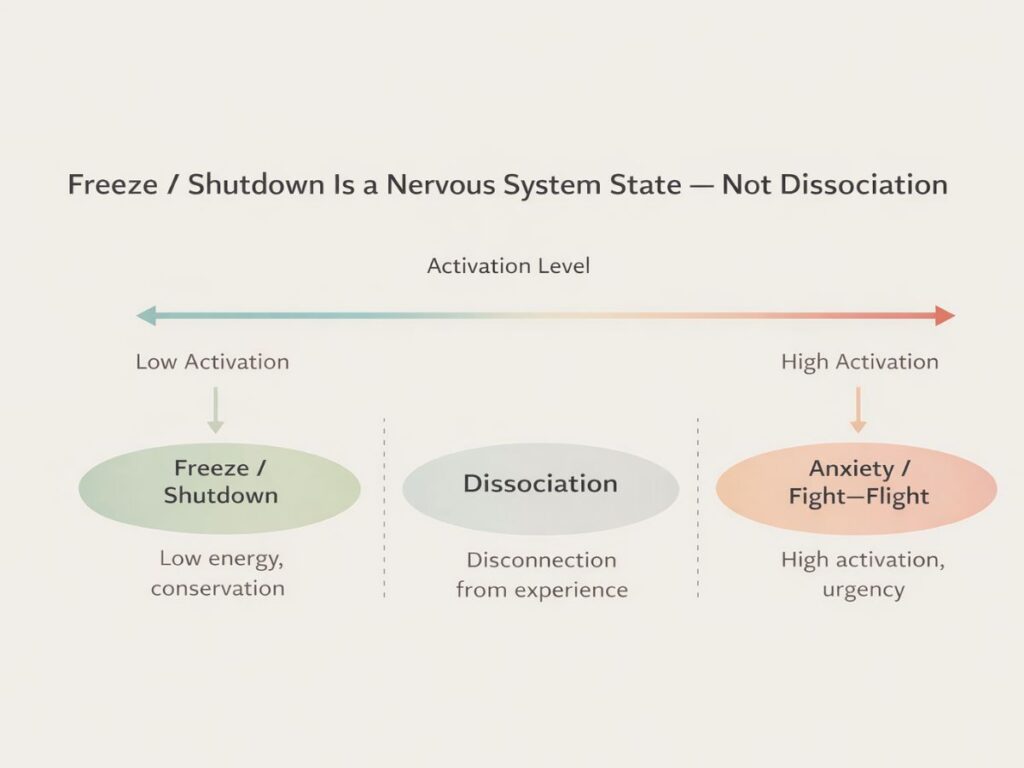
Shutdown vs. Dissociation — What’s the Difference?
Shutdown and dissociation can look similar, but they’re not the same. Shutdown is a whole-body nervous system state marked by low energy, heaviness, and reduced responsiveness. Dissociation involves mental or emotional detachment from yourself or your surroundings. Many people experience aspects of both, especially after chronic stress or trauma.
People often use shutdown and dissociation interchangeably because both involve some form of pulling away, even though they’re distinct experiences in the body.
What Shutdown Feels Like
Shutdown is primarily about energy conservation. The body slows things down. Movement feels harder. Speech may be quieter or delayed. Motivation drops because the system is trying to reduce output. You’re still here — just operating on low power.
What Dissociation Feels Like
Dissociation, on the other hand, is more about disconnection from experience. You might feel spacey, unreal, or as if you’re watching yourself from a distance. Your body may still be moving, but your sense of presence is disrupted.
Clinically, dissociation as a stress response involves a disruption in how a person experiences themselves or their surroundings, which is different from the low-energy, conservation-based state seen in shutdown.
Shutdown and Dissociation Often Overlap
A nervous system that has been under stress for a long time may move between shutdown and dissociation, or experience both at once. That doesn’t mean something new is wrong — it means your system has learned more than one way to reduce overwhelm.
Understanding the difference matters because what helps dissociation doesn’t always help shutdown — and vice versa.
This is often the point where people start to wonder why understanding their patterns hasn’t actually changed how they feel.
If you want to learn more about freeze states — including what a functional freeze can look like — you can read more about it in my blog on functional freeze.
Why Talk Therapy Alone Often Doesn’t Reach Shutdown
Talk therapy can be incredibly helpful, especially for understanding patterns, making meaning, and putting language to what you’ve been through. But shutdown isn’t a “thinking” problem or mindset issue. It’s a physiological state.
And research supports this, too. The American Psychological Association (APA) states that when stress persists without relief, the nervous system shifts its priorities toward conservation and survival rather than reflection or insight.
Why Insight Doesn’t Always Land in the Body
When the nervous system is in shutdown, access to emotion, memory, and motivation is already limited. So even when insights land intellectually, they don’t always register in the body. You might understand why you feel the way you do, but still feel flat, heavy, or disconnected afterward.
When Understanding Still Doesn’t Change How You Feel
This is where people often get frustrated. They’ve done the work. They can explain their history. They can name their triggers. And yet nothing feels different. That doesn’t mean therapy isn’t working — it means the system you’re trying to reach isn’t primarily operating through words.
Shutdown developed as a way to reduce load when activation felt unsafe or unsustainable. Asking a system in that state to analyze, reflect, or emote can unintentionally increase pressure rather than relieve it.
What Usually Doesn’t Help Shutdown
- Pushing yourself to “engage” or feel more motivated
- Processing emotions without body support
- Cognitive reframes that require energy you don’t have
These approaches assume the nervous system is resourced enough to respond. In shutdown, it often isn’t.
This doesn’t mean talk therapy is wrong or useless. It means timing and state matter.
When the nervous system is shut down, what helps most isn’t more insight — it’s less demand. Less expectation to perform insight, access emotion, or move forward before the body feels ready. Support needs to meet the system where it is, not where we think it should be.
This is why body-based therapy approaches are often more effective during shutdown. They work with sensation, pacing, and safety rather than relying on cognitive engagement that the nervous system may not have access to yet.
Approaches that include the body, such as pacing, sensation, safety, and gradual re-engagement, tend to be more effective for shutdown states. They don’t try to override the nervous system. They work with it.
How Somatic Therapy Helps When You’re Stuck in Freeze
Somatic therapy helps with shutdown by working directly with the nervous system rather than relying on insight alone. Instead of pushing activation, it focuses on safety, pacing, and gentle reconnection with the body. This allows energy, sensation, and responsiveness to return gradually, without overwhelming a system that learned to power down for protection.
Why Safety Comes Before Change
In a shutdown or freeze state, the nervous system isn’t waiting to be convinced — it’s waiting to feel safe enough to respond. Somatic therapy starts there.
Rather than asking you to analyze or explain what’s happening, the work focuses on what your body is already communicating through sensation, posture, breath, and pacing. The goal isn’t to activate you or “snap you out of it.” It’s to reduce threat enough that the system can begin to regulate on its own terms.
What Shifts Tend to Look Like Over Time
This often looks subtle from the outside. Small shifts in awareness. More access to sensation. Slight increases in energy or responsiveness that don’t feel forced. Over time, those shifts tend to feel steadier and easier to access.
For people stuck in freeze, this approach matters because it respects the original reason shutdown developed. It doesn’t override protection. It works with it slowly, safely, and with attention to timing.
This Isn’t About Forcing Yourself to Self-Regulate
Shutdown doesn’t shift by trying to relax harder or make your body feel calm. It changes when the nervous system experiences enough safety to re-engage without pressure or urgency.
When done well, somatic work doesn’t feel like effort. It feels like relief — not because something dramatic happens, but because the system is no longer being asked to do more than it can handle.
This is also why many people find that once their nervous system feels more calm, insight becomes more useful again. Understanding follows safety, not the other way around.
Is This Burnout, or Something Deeper?
Burnout usually improves with rest, boundaries, or time away. Nervous system shutdown often doesn’t. If exhaustion, numbness, or disconnection persist even after slowing down, it may reflect a deeper stress response shaped by chronic pressure or emotional overwhelm.
Burnout and shutdown can feel similar on the surface.
Both can involve fatigue, low motivation, and a sense of depletion. But they come from different places in the nervous system.
Burnout is typically the result of sustained output without adequate recovery. When the load is reduced, such as fewer demands, more rest, clearer boundaries, the body gradually rebounds. Energy returns. Interest comes back online. You feel tired, but still connected to yourself.
Shutdown feels different. Even when demands ease, the body doesn’t respond the way you expect. Rest doesn’t restore you. Time off doesn’t shift the fog. You might intellectually know you’re safe or supported now, but your system hasn’t caught up yet.
The Nervous System Conserves Energy
This is where people start blaming themselves. They wonder why they’re not “better” after doing all the right things. But shutdown isn’t a failure to recover — it’s a sign that the nervous system learned to conserve because stress once felt inescapable.
When pressure has been ongoing (relationally, emotionally, or internally) the nervous system may stay in low-power mode long after the external stressor has changed. Not because you’re weak, but because your body hasn’t yet experienced enough safety to stand back up. For some people, this pattern reflects the long-term effects of chronic stress (rather than situational burnout alone).
When to Consider Support
You might consider additional support if shutdown has been present for months, rest hasn’t changed it, or you feel increasingly disconnected from yourself or others. These are signs the nervous system may need help re-establishing safety, not more effort or discipline.

What Working With Me Looks Like When You’re Shut Down
If you come to work with me while you’re shut down, the goal isn’t to get you talking more, feeling more, or pushing through anything. We start by slowing the pace — not because you’re fragile, but because your nervous system has been working overtime for a long time.
Working With What Your Body Is Already Doing
Sessions are structured to reduce pressure from the start. That means we pay attention to how your body responds in real time: shifts in energy, changes in breath, moments where things feel heavier or lighter. We don’t rush past those cues. They matter more than insight in this phase.
You’re never asked to relive or rehash experiences before your system is ready. Instead, we work with what’s present — sensation, posture, attention, timing. The aim is to help your nervous system experience safety in the moment, not convince it that safety exists in theory.
What Change Tends to Look Like Over Time
Over time, people often notice small but meaningful changes. It becomes easier to stay present during conversations. Decisions require less effort. Rest starts to actually restore instead of just stopping the noise. These shifts tend to be gradual, which is exactly what makes them stick.
Most importantly, the work respects why shutdown showed up in the first place. There’s no assumption that something is wrong with you. The focus is on helping your system feel supported enough to come back to presence without being pushed or overridden.
Frequently Asked Questions About Shutting Down Under Stress
Is it normal to shut down when overwhelmed?
Yes. Shutting down when overwhelmed is a normal nervous system response, not a sign that something is wrong with you. When stress feels too intense or unrelenting, the nervous system may move into a low-energy, conservation state to reduce overload. This can show up as numbness, fatigue, foggy thinking, or a desire to withdraw — even if nothing looks “wrong” from the outside.
Why do I shut down when overstimulated?
Shutdown can happen when your nervous system perceives too much input with no clear way to resolve it. Sensory overload, emotional pressure, constant demands, or prolonged stress can all push the system beyond what feels manageable. When fight or flight no longer feel effective, the body may shift into shutdown to conserve energy and limit further strain.
Is shutting down a trauma response?
Shutting down can be a trauma-related response, especially for people who have experienced chronic stress, emotional overwhelm, or situations where escape or support wasn’t available. In those cases, shutdown develops as an adaptation. However, shutdown doesn’t always mean there’s unresolved trauma — it can also reflect how a nervous system has adapted to long-term pressure or overstimulation.
Ready to Feel Present Again?
If what you’re reading feels familiar, you don’t need to push yourself to “do something” about it right now. Simply recognizing shutdown for what it is — an evolutionary response, not a personal failing — can already take some pressure off your system.
When you are ready, support can help your nervous system move out of low-power mode at a pace that feels safe and respectful. The goal isn’t to force change, but to create enough stability that presence, energy, and responsiveness can return naturally.
If you’re curious about what that kind of work looks like, you can learn more about my approach to somatic therapy in Los Angeles and see whether it feels like a fit.




